15.11.23 (7)
Unnecessary screenings may lead to unwarranted stress, false positives, and harmful exposure—here’s why you might want to reconsider them.
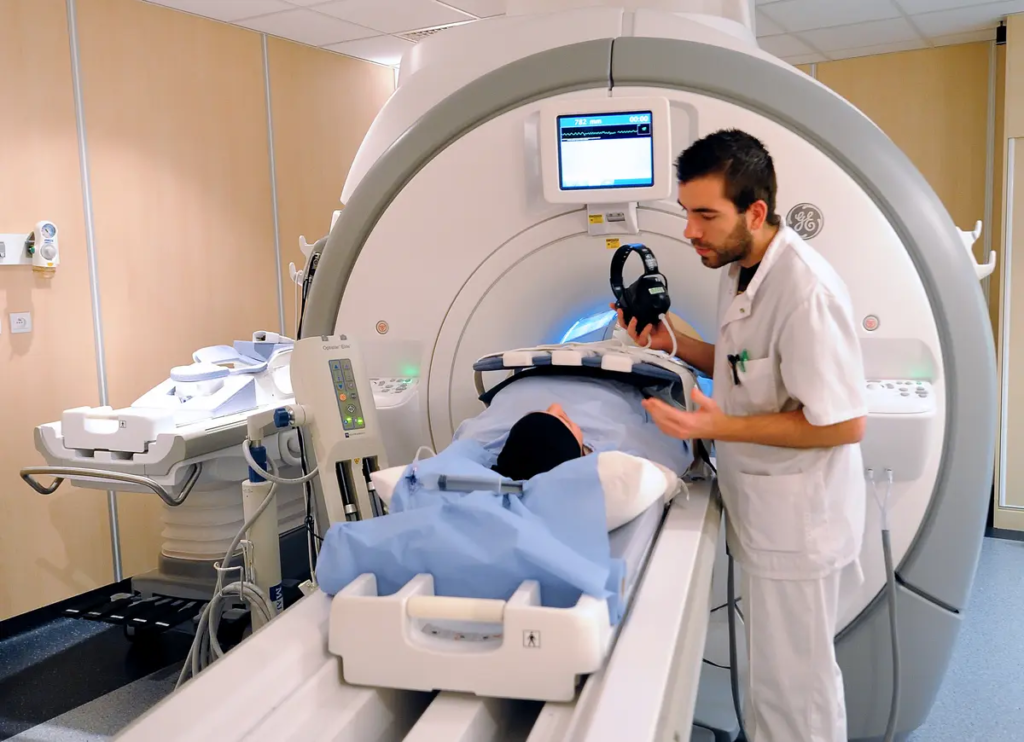
Are routine medical screenings always beneficial? Each year, millions of Americans willingly participate in these tests with the intent of safeguarding their health. Yet emerging evidence indicates that certain screenings may be unnecessary and even jeopardize people’s well-being.
The High Price of Excessive Medical Screening
The United States spends twice as much on health care per person as other industrialized nations, but the returns in terms of life expectancy are dishearteningly meager. Despite the high expenditures, the United States lags behind 12 high-income countries in numerous health indicators.
Although the United States is near the top of the list in screening rates for breast and colorectal cancer, behind only Sweden and the Netherlands, the efficacy of such frequent screenings is debatable.
“Over-testing is at the root of many of our problems,” Dr. Jerome Greenberg and Dr. Jonas B. Green wrote in an American Journal of Medicine commentary highlighting that there are opportunity costs in ordering, reviewing, and explaining tests.
“When a test isn’t unnecessary, time can be more appropriately spent counseling patients, listening to them, and redoubling efforts to follow well-supported preventive guidelines.”
A recent JAMA review reveals that up to $935 billion in annual health care spending is wasted, a substantial portion resulting from unnecessary tests or procedures.
Dr. Greenberg and Dr. Green highlight five key reasons clinicians over-test: They believe that tests may detect subclinical disease, they want to practice defensive medicine, they lack knowledge or confidence, the patient expects it, and profit.
Over-screening carries a significant economic burden, but its human cost is even more profound. Unwarranted tests can result in anxiety, false alarms, and harmful exposures. Dr. Greenberg and Dr. Green emphasize that the drawbacks—low diagnostic yield, high costs, and the emotional strain of false positives—are often overlooked when prescribing screenings for people who are asymptomatic.
7 Tests You May Not Need and That May Even Cause Harm
1. Cardiac Stress Test
Cardiac stress tests, commonly used to identify coronary artery disease (CAD), require patients to exercise on treadmills or stationary bikes as their heart rate and blood pressure are observed.
Occasionally, doctors who want a closer look may recommend a nuclear stress test, during which a radioactive substance is used to visualize the heart, exposing patients to radiation equivalent to that of about 400 chest X-rays. Eight million of these tests are performed in the United States each year.
Despite their prevalence, the reliability of these tests for indicating heart health is under scrutiny. Experts point out that a stress test mainly “detects only significant coronary stenosis and does not identify nonobstructing plaques,”—a common cause of heart attacks. Thus, an “all-clear” from such tests could be misleading.
Inaccurate stress test results have considerable consequences—nearly 3 percent of recipients undergo additional procedures, and 1.7 percent experience severe adverse reactions; these are often people without CAD.
A study in the Annals of Internal Medicine amplifies this concern, estimating that unnecessary cardiac stress tests, particularly those involving imaging, cost the U.S. health care system $501 million annually and could lead to about 500 cancer cases yearly.
Cardiac stress tests are best reserved for symptomatic patients or those at high risk of disease. Recent advice from the American College of Cardiology recommends against routinely using imaging stress tests to investigate common symptoms such as heart palpitations or feeling faint.
2. Coronary Calcium Scan
Coronary artery calcium (CAC) scans aim to detect calcium, a plaque component, in the heart’s arteries and thereby identify early signs of CAD. Despite becoming more common, the effectiveness of CAC scans in preventing cardiovascular events remains contested.
Although calcification can suggest a risk of cardiac events, the test fails to identify soft or noncalcified plaques, which can rupture and cause heart attacks. Therefore, relying exclusively on calcium scoring could underestimate the risk of CAD.
In an editorial, Dr. John Mandrola and Dr. Andrew Foy wrote, “Potential harms from coronary artery calcium testing include radiation exposure … incidental findings in up to 40% of scans, misdiagnosis, and downstream testing.”
For patients at both low and high risk of CAD, a coronary artery calcium score may not offer meaningful, actionable insights. Dr. Mandrola and Dr. Foy wrote, “Atherosclerosis [a buildup of plaque in the arteries] is a complex lifelong disease, and wrongly simplifying it with coronary artery calcium testing helps the testers more than the tested.”
Coronary calcium scans best serve high-risk individuals or those experiencing symptoms of CAD.
3. CT Scan or MRI
Diagnostic imaging has proven invaluable in detecting and treating various health conditions early. Yet, with the United States conducting 245 computerized tomography (CT) scans and 118 magnetic resonance imaging scans (MRIs) per 1,000 people, it surpasses the usage rates of most developed countries.
Despite their merits, these scans aren’t without drawbacks. A common issue is what experts describe as “radiographic incidentalomas,” incidental findings that present little risk. These unexpected abnormalities can lead to unnecessary additional tests, treatments, and anxiety for patients.
CT scans expose patients to radiation, equivalent to 70 times that of a chest X-ray, potentially contributing to thousands of cancer cases annually. Additionally, concerns have arisen regarding the contrast dyes used in these scans, which may cause allergic reactions, leave trace deposits in the brain, or lead to severe neurological problems such as those seen in gadolinium deposition disease.
The frequent reliance on these scans can result in a high number of false positives. For instance, although 95 percent of scan recipients may receive abnormal results, less than 2 percent of these results point to malignant cancers.
In the past decade, there has been a surge in people seeking whole-body CT scans or MRIs for early disease detection. Nonetheless, in April, the American College of Radiology warned, “There is no documented evidence that total body screening is cost-efficient or effective in prolonging life.” They, along with other experts, alert the public to the risks of unnecessary procedures and stress.
4. Bone Density Scans
Bone density scans, known as dual-energy X-ray absorptiometry scans, are a common tool for assessing osteoporosis risk by measuring bone loss in the spine, hips, and wrists. Despite their utility, particularly for postmenopausal women and people with a history of fractures or osteoporosis risk factors, research questions the necessity of their routine use across the broader population.
A study involving 6,150 women revealed that many osteoporosis drug prescriptions may be unnecessary and based on potentially unreliable bone density scans. Notably, two-thirds of these prescriptions were based on scan abnormalities not recognized by international guidelines as definitive proof of osteoporosis, with half given to younger women without risk factors.
The scans employ a minimal amount of ionizing radiation, much less than a chest X-ray or a CT scan. While generally considered low risk, radiation exposure adds up. Incidental findings, or unrelated abnormalities picked up during the scan, may also lead to further tests, costs, and anxiety for the patient.
5. Colonoscopies
The colonoscopy is celebrated as a highly accurate diagnostic tool for detecting colorectal cancer, consistently proving its ability to identify the disease early.
Most people are advised to begin colon cancer screening at age 45. If no adenomas or cancer are found, and there are no risk factors, the next screening is usually scheduled 10 years later—although this guideline isn’t always followed.
A study found that of more than 24,000 patients with precise colonoscopy results, nearly half underwent another test within seven years despite no clear indication of risk.
Despite their importance for early detection, colonoscopies carry risks including heavy bleeding, colon tears, diverticulitis, and abdominal pain. For those with cardiovascular issues, complications can occasionally lead to treatments such as blood transfusions, surgery, or hospitalization, and though it’s rare, may even be fatal.
A recent study published in The New England Journal of Medicine questions the perceived benefits of colonoscopies, suggesting that their effectiveness in reducing cancer deaths might have been overestimated.
Less invasive alternatives for colorectal cancer screening exist. The fecal immunochemical test detects hidden blood in stool samples with 80 percent accuracy. Similarly, the Cologuard test searches for atypical DNA and blood traces, indicating potential precancerous polyps or colorectal cancer.
6. Prostate Screening Test
Routine for men’s health checks, prostate cancer screenings are being reevaluated for their necessity following recent findings. The commonly used prostate-specific antigen (PSA) test is under scrutiny amid concerns that it may do more harm than good.
Nearly 70 percent of men age 70 to 80 have some cancer cells in their prostate, though not all cases warrant concern. The American Academy of Family Physicians asserts that PSA-based screenings frequently identify benign tumors, potentially leading to unnecessary and risky treatments.
A concerning trend was highlighted in a JAMA study: Between 2016 and 2018, 38 percent of men aged 70 and older received low-value PSA screenings. More than half of these men underwent follow-up services, primarily repeated PSA tests, leading to undue stress, medical procedures, and significant financial costs—$6 in follow-up care for every $1 spent on initial screening.
Doctors are now urged to reconsider ordering PSA screenings and to discuss the risks and benefits comprehensively with patients. The aim is to base screening decisions on each individual’s unique risk factors, averting unnecessary treatments and ensuring optimal care.
7. Pap Smears
Although cervical cancer screenings are life-saving, there is concern over potential over-testing. A recent JAMA study indicates excessive use among women at average risk.
Despite evolving guidelines, cervical cancer screening remains excessive. One study revealed that nearly 10 million women who had a hysterectomy and weren’t at risk for cervical cancer had received unnecessary Pap smear screenings.
“If there was no potential for harm from screening, it would not be unreasonable to do more frequent testing,” Dr. Jason D. Wright, senior author of the study, said in a press release. “The issue is there are real downsides to over-screening.”
The American College of Obstetricians and Gynecologists provides clear guidance: Pap smears aren’t advised for women under 21, as most cervical abnormalities in this group self-correct, making the tests unnecessary and potentially stressful. Similarly, women older than 65 with a 10-year history of negative results need not undergo Pap smears.
Women aged 21 to 29 should have a Pap smear every three years. Those aged 30 to 65 can choose from a Pap smear every three years, an HPV test every five years, or both tests concurrently every five years.
Choosing Wisely
Initiated by the American Board of Internal Medicine Foundation, the “Choosing Wisely” campaign aims to reduce unnecessary medical tests and procedures. It encourages patients and health care providers to engage in informed discussions. Since its launch in 2012, the campaign has devised a list of five questions to ask your doctor before undergoing any test, treatment, or procedure:
“Do I really need this test or procedure?” “What are the risks?” “Are there simpler, safer options?” “What happens if I don’t do anything?” “How much does it cost?”
Though collaboration between patients and doctors is crucial in deciding the necessity of a test, physicians may not always have the latest recommendations at their fingertips. Hence, the onus often falls on patients to do their homework. Choosing Wisely is a resource for patients seeking to understand the utility and implications of various tests and treatments.
In this context, asking a simple question—”What will I do with this information?”—becomes vital when considering any test. It’s a checkpoint ensuring that the decision isn’t just clinically valid but is also aligned with a patient’s unique situation and needs.
Thanks to theepochtimes.com